
Coronavirus
Technology Solutions
July 21, 2021
The Merits of
Indoor Mask
Wearing
Better Mask High
Filtration
System
Combines
Safety and
Comfort
Armbrust
American
Compares Mask
Efficiency
Mask Mandates
are Likely for
Many Areas
Western Wildfire
Smoke Creating
Serious
Air Problems in
Philadelphia
Manitoba Relying
on Upgraded HVAC
to Keep Children
Safe
Better Home
Ventilation Now
is a Goal of
Many Residents
______________________________________________________________________________
The Merits of
Indoor Mask
Wearing
The chances of
dying from COVID
over the last
year were 0.17%.
Your
chances of dying
in a car
accident were
1/20 of that
number or
0.008%.
We could avoid
riding in cars
but the quality
of life benefits
outweigh the
risks. With a
risk level of
COVID continuing
throughout your
life you
statistically
will lose 14
years of life.
In contrast
avoiding
automobile
travel would
only add 6
months to your
statistical
life. In
principle people
could
choose solitary
confinement and
a rigid health
regime and live
to be 100. But
no one would
choose this
option compared
to living to 80
and enjoying
life.
Before the Delta
variant became
dominant and
while we thought
we could achieve
the 70-80%
totally
vaccinated rate
the expectation
was that we
would reduce the
risks to less
than 6 months of
life reduction.
We now have to
assess the
situation in
light of the
variant and half
the population
not being
vaccinated.
There is one
risk for
vaccinated
people and one
for
unvaccinated.
For the
unvaccinated the
potency of the
Delta variant
offsets the
benefits of the
50% vaccination
rate.
This means that
in an indoor
setting the
unvaccinated
will continue to
face a
statistical life
reduction of 14
years. The
vaccinated
person has 90%
protection so
without masks he
still faces a
risk of 1.4 year
life reduction.
Another way to
look at this is
by living a
normal life
rather than one
in solitary you
lose 20 years.
Another 1.4
years is not an
enormous amount.
However, the 20
year sacrifice
covers all the
good food,
social activity,
and benefits of
modern living.
It would be a
small
comparative
reduction in
life quality to
wear a highly
efficient mask
in public indoor
settings. This
would add
another 90% in
protection and
reduce the risk
to 0.14 years.
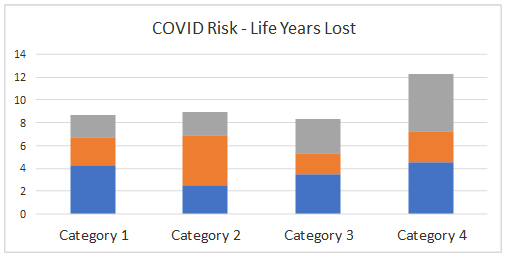
Normal pleasures
reduce life
expectancy from
100 to 80. But
this added risk
for the
unvaccinated
reduces
expectancy to 66
years. On the
other hand if
you are
vaccinated and
wear a mask
indoors and in
public spaces
you only reduce
life expectancy
by two months.
This is a
minimal risk and
should not
impact
normal
business and
social activity
for those who
take the
precautions.
For the
unvaccinated it
will be
important to
mandate masks
which would also
bring down risks
to the 1.4 year
loss level.
This comparison
has been based
on a whole life
led at a given
risk level. So,
the 20 years of
normal life lost
is an
accumulation of
thousands of
desserts, years
of driving, and
many other hours
of enjoyment.
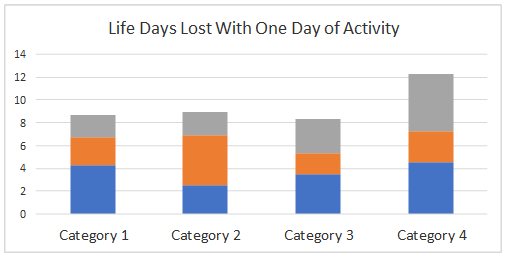
If one focuses
instead on
whether to
attend a single
event such as a
wedding or
parade a
different
picture is
created. The
risk could be
800 times
greater than
that of a normal
day. Some events
are worth the
high risk.
Millions of
soldiers have
died with this
belief.
Astronauts
willingly take
high risks.
A complicating
factor is risk
to others. Small
children cannot
be vaccinated
and are at risk
if adults are
not vaccinated.
Better Mask High
Filtration
System
Combines
Safety and
Comfort
America is
opening back up
again. With air
travel,
conferences, and
workplaces
returning. The
Better Mask Kit
is claimed to be
the best
solution for
protecting
yourself, your
coworkers, and
your fellow
travelers as you
enter the new
normal.

The three most
important things
to consider when
choosing a mask
are:
Fit: How
well does the
mask seal?
Filtration:
What level of
protection does
the mask
provide?
Comfort:
How long can you
wear the mask?
By combining the
superior
filtration of
an Armbrust filter with the customizable seal provided
by an FTM
Essential Brace,
The Better Mask
is a marriage of
form and
function
designed to
provide
comfortable,
high-level filtration
with a better
seal around the
face.

The brace's
patent-pending
nose cushion
applies light
pressure for a
superior fit
with minimal
leakage for any
face shape,
while the
filtration
provided by the
Armbrust filter provides
a 98%
filtration of
particles as
small as .01
micron.
Armbrust
American
Compares Mask
Efficiency
Particulate
Filter
Efficiency (PFE)
is the standard
by which masks
are evaluated.
Armbrust
American has
conducted
comparison tests
of various
masks. It tests
to the ASTM
standard using a
PFE machine to
blow .01 micron
latex particles
through a mask
at an airflow of
85L/min in order
to max out the
mask’s filter.
The machine then
uses optical
scanning
technology to
report how many
particles slip
through.
Tests results
for many
suppliers in
China, the U.S.
and elsewhere
are provided.
There is
a wide range in
efficiencies
https://www.armbrustusa.com/pages/mask-testing
Mask Mandates
are Likely for
Many Areas
Two months after
the Centers for
Disease Control
and Prevention
said vaccinated
individuals
didn’t need to
wear masks in
most settings, a
growing number
of experts are
warning it’s
time to put them
back on.
First, there was
Los Angeles
County, where
the rising
menace posed by
the delta
variant of the
coronavirus
prompted health
officials to
reimpose a mask
mandate. Then,
Bay Area health
officers on
Friday
recommended that
residents of
seven counties
and the city of
Berkeley,
Calif., resume
wearing masks
indoors. Mask
mandates are
being discussed,
too, in
coronavirus hot
spots such
as Arkansas and Missouri,
where cases have
sharply
increased in
recent weeks and
many residents
remain
unvaccinated.
“Universal
masking indoors
is a way of
taking care of
each other while
we get more
people
vaccinated,”
said Barbara
Ferrer, director
of the Los
Angeles County
Department of
Public Health,
which last week
moved
to reinstate an
indoor mask
mandate. “It
really doesn’t
disrupt any
business
practices. It
allows us to
remain fully
open — while we
acknowledge that
the delta
variant [is]
spreading like
wildfire here.”
Los Angeles
County said July
15 it will
reimpose indoor
mask mandates as
coronavirus
cases linked to
the delta
variant
continued to
rise among the
unvaccinated.
(Reuters)
And the nation’s
current and
former surgeon
generals warned
the nation
should brace for
a broader return
to mask-wearing.
“We need to
prepare the
public for what
could be, again,
a return to some
of these
mitigation
measures,”
former surgeon
general Jerome
Adams told
Indianapolis TV
station
WISH-TV on
Sunday,
highlighting a
resurgence of
the virus across
the Midwest.
Adams, an
appointee of
former president
Donald Trump,
called on the
CDC to “hit the
reset button”
and once again
recommend
widespread
mask-wearing as
coronavirus
cases spike.
But the growing
calls to
reinstate mask
mandates —
echoed by the
American Academy
of Pediatrics,
which Monday
called for
everyone over
the age of 2 to
wear masks,
regardless of
vaccination
status — renewed
a cultural and
health flash
point a year and
a half after the
virus landed in
the United
States.
“We need to be
reopening our
state, not
reimposing
unnecessary
restrictions,”
Kevin Faulconer,
the Republican
former San Diego
mayor now
running for
California
governor, wrote
on Twitter last
week. The Los
Angeles County
sheriff last
week said he
would refuse to
enforce the
local masking
mandate, and
Republicans
nationally took
aim at existing
protections.
The daily
average of
confirmed U.S. coronavirus cases
has nearly
tripled in the
past month, from
fewer than
12,000 on June
19 to almost
35,000 on
Monday,
according to The
Washington
Post’s seven-day
average of
coronavirus
cases. Experts
on coronavirus
transmission say
masks remain a
crucial tool to
protect tens of
millions of
unvaccinated
Americans — and
even vaccinated
people, with
growing evidence
of breakthrough
infections in
some fully
immunized
adults, although
health officials
have said most
people who have
died or been
hospitalized
with covid-19 in
recent weeks
were
unvaccinated.
“The best
protection
everybody has is
masks,” said
Kimberly
Prather, a
professor at the
University of
California at
San Diego who
has studied
airborne virus
transmission and
said she
“absolutely”
supports the
resumption of
indoor mask
mandates.
Prather said she
has also grown
wary of going
without a mask
in some settings
outside, warning
that the delta
variant is
hyper-transmissible.
The delta
variant has
become the
dominant strain
of coronavirus
in the United
States resulting
in a rise in
infections and
hospitalizations.
(John
Farrell/The
Washington Post)
“While delta
numbers are
going up — and
if I’m in a
crowded outdoor
location with
lots of people
yelling — I
would be wearing
a mask,” Prather
said.
But many
Americans say
they have
stopped wearing
face coverings,
and experts
acknowledge it
will be
difficult to
persuade them to
resume.
“I think people
will be
disappointed
that folks were
having some hope
and seeing the
light at the end
of the tunnel —
and this would
be a suggestion
that we’re
taking a step
back,” said
Marcus Plescia,
chief medical
officer at the
Association of
State and
Territorial
Health
Officials.
Just 55 percent
of respondents
to an Axios/Ipsos
poll in late
June said they
were wearing
masks
“sometimes” or
“at all times”
in public, down
from 68 percent
who said the
same in early
June and nearly
90 percent in
February, March
and early April.
Plescia said he
supports the
resumption of
local mask
mandates, given
the rise in
cases and the
growing evidence
about the threat
of the delta
variant.
“You know,
recovery from
just about
anything comes
in cycles —
things get
better, and they
get worse, and
they get better,
and they get
worse. It’s rare
that it’s
linear. And I
think that’s
what’s going on
here,” Plescia said.
Some physicians
who embraced
mask mandates
last year said
they’re
concerned the
moment has
passed.
Former Louisiana
health
commissioner
Rebekah Gee, who
is CEO of Health
Care Services
for LSU
Health, wrote
last year that
she favored the
use of mask
mandates to
protect public
health. But “at
this point, I’m
not convinced
that requiring
masks in every
aspect of
society is
effective,” Gee
said Monday,
warning that
many Americans
had tuned out
public health
officials’ calls
to wear masks
and take other
steps to guard
against the
coronavirus.
Gee instead said
she favors
targeted mask
requirements,
such as
mandating use in
close quarters
or when
interacting with
vulnerable
populations such
as children
younger than 12,
who have yet to
get vaccinated.
Gee also said
she supports
private-sector
requirements for
masks.
The pace of
vaccinations has
steadily
declined from
about 2 million
shots per day in
mid-May to fewer
than 550,000
shots a day.
Health
officials’ goal
of ensuring that
at least 70
percent of
adults receive
one shot of a
vaccine, which
President Biden
initially
targeted for
July 4, is
unlikely to be
reached before
Aug. 10,
according to The
Post’s projections.
Federal
officials have
defended the
CDC’s earlier
decision on
mask-wearing. In
a Washington
Post
Live interview
Monday, National
Institutes of
Health Director
Francis S.
Collins said the
CDC’s
recommendations
for fully
vaccinated
people to remove
their masks were
issued before
the delta
variant began
broadly
circulating —
and before it
was clear how
much vaccine
hesitancy would
exist in some
parts of the
country.
“I know people
are tired of
masks, but it’s
not so awful to
consider having
to put a cloth
mask on your
face when you’re
inside if it’s
going to
potentially stop
what is, right
now, looking
like a pretty
significant
surge of
infections,
especially in
places where
vaccination
rates are low,”
Collins said.
Surgeon General
Vivek H. Murthy
said the federal
government
supports local
mask mandates in
places where
cases are
surging or many
residents are
unvaccinated.
“It’s very
reasonable for
counties to take
more mitigation
measures, like
the mask rules
that you see
coming out in
L.A.,” Murthy
said Sunday on
ABC News’s “This
Week.” “I
anticipate that
will happen in
other parts of
the country,
too.”
https://www.washingtonpost.com/health/2021/07/19/mask-mandates-returning/
Western Wildfire
Smoke Creating
Serious Air
Problems in
Philadelphia
Smoke from the
massive
wildfires
burning in
Oregon and
Canada has
drifted over the
Philadelphia
region in recent
days, causing a
high level of
pollution that
could pose a
health threat to
those with
conditions like
heart disease,
asthma, and
emphysema. It
even can affect
the immune
system -- making
an encounter
with the
coronavirus more
dangerous.
Can those masks
you’ve been
wearing to
protect against
COVID-19 help?
The simple
answer: It
depends on the
mask. But it
helps first to
understand what
the masks are up
against.
Both Tuesday and
Wednesday,
Philadelphia
declared a Code
Orange pollution
action day for
fine particles
because of high
readings due to
the wildfires.
The Pennsylvania
Department of
Environmental
Protection also
issued a Code
Orange alert for
Bucks, Chester,
Delaware, and
Montgomery
Counties because
of the smoke.
The city’s
overall air
quality was
listed at 145
Wednesday
morning, which
is in the range
interpreted as
unhealthy for
sensitive groups,
according to
Philadelphia
Department of
Public Health
spokesperson Jim
Garrow. That
could change if
a cold front
moves through as
expected,
bringing
thunderstorms.
However, the
level of PM2.5
on Tuesday
reached 53.5
micrograms per
cubic meter, far
in excess of the
federal
Environmental
Protection
Agency’s
National Ambient
Air Quality
Standard of 35
for a daily
reading. It was
likely only the
second time in
the last five
years levels
have reached
that high,
however that has
not yet been
officially
determined.
“People who have
heart and lung
problems may
experience some
health effects
and should limit
their time
outdoors,”
Garrow said.
“The general
public is
considered to be
much less likely
to be affected.”
The pollutant
from the
wildfire smoke
is known as
PM2.5, for the
very fine
particulate
matter it
contains,
defined as
concentrations
of 2.5 microns
or smaller.
These particles
are so small —
far smaller than
the width of a
human hair —
that they are
easily inhalable.
The World Health
Organization
says PM2.5 is
responsible for
the biggest
proportion of
health effects
from air
pollution.
Normally, the
biggest local
sources of PM2.5
are emissions
from gas- and
diesel-powered
vehicles. Power
plants are also
a source. The
particles form
when emissions
react in the
air.
Health effects
can stem from
short or long
exposure and can
range from
aggravation of
asthma and other
respiratory
illnesses to
premature death
in people with
chronic heart or
lung diseases.
Children and
seniors are most
vulnerable.
The worst season
for pollution in
Philadelphia is
typically
summer. So, the
wildfires are
adding to what
is already a
difficult
situation.
The federal
Centers for
Disease Control
and Prevention
says that
wildfire smoke
can irritate
lungs, cause
inflammation,
affect immune
systems, and
make people more
prone to lung
infections,
including the
virus that
causes COVID-19.
Russell Zerbo,
an advocate with
the Clean Air
Council, said
a volunteer
network of air
monitors
across the
region is
recording the
highest levels
of PM2.5 that
he’s seen on a
sustained basis.
“I’ve never seen
such universally
high numbers for
PM2.5 in
Philly,” Zerbo
said. “You can
see we are at
the center of
where this is
drifting across
the country. New
York is getting
lower readings.
North Carolina
is getting lower
readings. So
this cloud is
really affecting
the
Philly-D.C.-Baltimore
area.”
Zerbo says N95
masks were made
to help
construction
workers filter
out the fine
particles
emitted during
demolition and
other hazardous
work, and so
will help with
wildfire smoke.
The CDC agrees,
noting that
cloth masks, or
regular surgical
masks, will not
protect people
from the
particulate
matter
associated with
smoke. Cloth
masks
do help slow the
spread of
COVID-19 by
blocking
respiratory
droplets but are
not designed to
catch the very
small, harmful
particles from
wildfire smoke.
The CDC notes
that medical
workers are the
ones who most
need access to
N95 masks. So it
recommends using
KN95 respirators
that are most
commonly made in
China and
similar to N95
masks. It
cautions,
however, that
buyers should
look for KN95
masks that meet
requirements
similar to those
set by the CDC’s
National
Institute for
Occupational
Safety and
Health for
respirators.
https://www.inquirer.com/health/coronavirus/wildfire-smoke-philadelphia-breathing-covid-masks-20210721.html
Manitoba Relying
on Upgraded HVAC
to Keep Children
Safe
With vaccines
ramping up and
COVID-19 cases
going down,
200,000 people
in Manitoba are
under the age of
12 — nearly 15
per cent of the
province's
population — and
still don't
qualify for a
coronavirus
shot, putting
the pressure on
school divisions
to make sure
classrooms are
safe.
Out of the
province’s 37
school
divisions, 33
tell Global
News they've
been increasing
filter changes
or have made
adjustments to
their HVAC
system.
"Even if
vaccines became
available for
the next age
group, five to
12, that
wouldn't be
until the fall.
And then you're
looking at a
month to two
months at least
before they have
full immunity.
So these next
few months, the
students are at
risk," said
Winnipeg
physician Dr.
Lisa Bryski.
"We don't want
to take chances
with people who
are vulnerable
and put them in
a population
density of a
classroom
without
vaccines."
One way to keep
classrooms safe
is to look into
schools'
ventilation,
according to
Jeffery Siegel,
a professor in
the department
of civil and
mineral
engineering at
the University
of Toronto.
"Ventilation is
enormously
important for
respiratory
disease
transmission,"
said Siegel.
He recommends
schools take a
multi-layer
approach.
"We should
absolutely be
addressing
ventilation,
filtration in
those spaces,"
he said.
"We know that
some people
don't wear masks
very well. We
know that not
everyone can be
vaccinated. We
know that
sometimes you
can't put in as
good a filter as
you want or you
don't have
enough HEPA
filters for the
classroom.
"So the idea is
you want to get
as many of these
layers as
possible."
To have a
properly
ventilated
classroom,
Siegel said
there should be
six air changes
every hour.
Turnover that is
as low as one or
two is not good
enough, as
particles can
remain in the
air for too
long, he added.
"A lot of
contaminants in
the space, as
well as
respiratory
virus particles,
can linger for a
long enough
period of time
that we're
seeing a higher
risk of
infection."
Opening windows
can help, he
said, but there
are a lot of
varying factors.
With vaccines
ramping up
and COVID-19 cases
going down,
200,000 people
in Manitoba are
under the age of
12 — nearly 15
per cent of the
province's
population — and
still don't
qualify for a
coronavirus
shot, putting
the pressure on
school divisions
to make sure
classrooms are
safe.
Out of the
province’s 37
school
divisions, 33
tell Global
News they've
been increasing
filter changes
or have made
adjustments to
their HVAC
system.
Better Home
Ventilation Now
is a Goal of
Many Residents
COVID-19 has
changed so many
of our
behaviors,
from how we deal
with
germs to how we
deal with
people. It has
altered the way
we work and the
way we view our
homes. It has
even made us
rethink the air
we breathe.
Prior to the
pandemic, air
quality was
something people
generally talked
about in the
context of air
pollution or
seasonal
allergies. That
all changed over
the past year.
"A year ago,
many people
weren't all that
interested in
air quality,"
says Ted Myatt,
ScD, a senior
environmental
scientist at
Environmental
Health and
Engineering,
Inc., who has
spent 20 years
studying
environmental
science. "It's a
really important
issue people are
just now
understanding;
it's important
to think about
what you are
exposed
to-especially in
your own home."
According to a study
by the EPA conducted
pre-COVID, we
spend 90 percent
of our time
indoors, and
that has likely
increased with
the pandemic,
especially as
more companies
commit to the
work-from-home
model
permanently.
Although indoor
air quality may
not be as
visually
rewarding as a
new countertop
or wood floors
in our houses,
it's an
important
consideration
that can
influence the
health of our
homes and
families. We do
know that air
filters and
purifiers can
help with
allergens,
and we are still
learning about
their role in
the spread of
viruses, like
the coronavirus
that causes
COVID-19. As
interior
designers,
homeowners, and
apartment
dwellers begin
to better
understand the
relationship
between air
quality and our
health, here are
a few things the
pros recommend
focusing on as
we move forward.
In the past,
most of us
focused on the
heating and AC
side, but during
the pandemic,
the
"ventilation"
part became top
of mind.
Essentially, the
HVAC in your
home is a system
for circulating
air between
indoor and
outdoor spaces.
An HVAC
professional can
inspect the
system by
measuring
factors like air
exchange rate,
or how often the
air in a room is
replaced with
fresh air, to
determine if
it's time for an
updated system.
In addition to
potential health
benefits, there
are also
environmental
and financial
reasons to
upgrade your
HVAC system.
"These days,
modern AC units
are more
efficient and
kinder to the
environment than
those many
homeowners may
have purchased
over the last 15
or 20 years,"
says interior
designer Breegan
Jane, who has
been working
closely with
HVAC company Trane
Residential to
help best advise
her clients.
"Upgrading your
HVAC system is a
great way to
start adding
value to your
home," she says,
if you are
looking to
eventually sell.
A new HVAC
system can cost
a ton of money,
so if that's not
in the cards,
commit to the
upkeep of what
you have. Jane
says that even
regular checks
can go a long
way. "Your HVAC
system's filters
should be
cleaned every 30
to 90 days-not
once a year, as
we tend to
think, to ensure
optimal indoor
air quality,"
she says. Air
filters are
designed to
capture all of
the yuck:
dander, dust,
allergens, etc.
If we aren't
cleaning them,
they can't do
their job. The
same logic
applies to air
purifiers, too.
The air
filtration needs
in a high rise
apartment
building will be
different than
in a single
family home, and
the needs may
even vary from
room to room in
your own house
if you are
considering a
portable air
purifier.
"Since an
apartment is
likely smaller
than a house, an
air purifier
will be even
more effective
there in
removing germs,"
says interior
designer Emma
Beryl. Plus, a
portable air
purifier may be
the only option
in an apartment,
where you don't
have the same
control over a
full building
airflow
redesign. "Think
of it as another
tool in the
toolbox to
mitigate
exposure," says
Myatt.
HEPA filters are
certainly the
gold standard,
but you'll also
want to check
how much square
footage the
filter can
cover. For
example, if your
filter is rated
for 150 square
feet and you
place it in a
250-square-foot
room, you're
only getting
partial
coverage. Check
out our
guide to the
various types of
filters available
and where they
might work best.
There is a
reason that
COVID-19 experts
said socializing
outside was
safer than
indoors and the
CDC recommended
opening your
windows for
increased
airflow if you
were having
people inside.
Air stagnation
correlates to
poor air
quality.
Even if you
can't update
your HVAC system
or your older
building isn't
equipped with
one, the CDC
offers some easy
ventilation
mitigation
strategies.
The simplest
solution? Open
the windows.
Opening a window
or door will
introduce more
outdoor air,
preventing stale
air from
circulating
around the room.
Using fans,
especially when
placed
strategically,
can also help
boost the power
of open windows.
For example, a
window fan can
be used to
exhaust indoor
air outside.
Opening our eyes
to indoor air
quality issues
in our own homes
may also prompt
us to consider
the air quality
in our schools,
office
buildings,
restaurants, or
other public
spaces. When
debating whether
to reopen
schools during
the pandemic,
inspections of
air filtration
systems in
schools became a
large focus. And
even before the
pandemic, one
study in Los
Angeles questioned
whether the
installation of
air filters in
schools could
significantly
boost the
student's test
scores.
While the link
between air
quality and test
scores is still
up for debate,
the correlation
between air
pollution and
worse asthma
symptoms has
been evidenced
in numerous
studies, again
highlighting air
quality as a
public health
issue. Whether
the concern is
the spread of
airborne
diseases,
pollutants, or
allergens, an
increased focus
on and demand
for improved air
filtration in
our public
spaces has been
sparked.
https://www.realsimple.com/home-organizing/home-improvement/maintenance-repairs/home-air-filtration
