
Coronavirus Technology Solutions
May 14, 2020
Masks for Everyone Who Ventures
Outside Each Day
The Coronavirus may Become
Endemic like HIV
Berry Installing New Meltblown
Line in Berlin
Nursing Homes are Starting to
Incorporate HEPA Filters and
Antimicrobial Coatings
UV Light for Jails and Nursing
Homes
Washington State Dental Office
will Open with New Air Filters.
Northwestern Professor looking
at Chemically Treated Masks to
Destroy Viruses
Ben Gurion University
Researching the Potential for
Electrically Charged Graphene
Graphene also being pursued by
Hong Kong Polytechnic
Carbon Nanotubes are Another
Option
Masks with Copper Technology
Offered by Multiple Companies
___________________________________________________________________________
Masks for Everyone Who Ventures
Outside Each Day
The expert opinion on the value
of masks to fight COVID is
nearly the opposite of what it
was earlier in the year. Studies
show that nations which require
people to wear masks do much
better than those who do not.
The deaths per capita in the
U.S. are 70 times greater than
China. Because of air pollution
China has a long history of mask
wearing. Japan never shut down
but has a low death rate. The
reason is that the wearing of
masks is universal.
The latest discoveries are that
a significant fraction of the
virus travels in small aerosols
similar in size and mobility to
cigarette smoke.

A surgical mask may stop the
larger droplets caused by
sneezing and coughing but not
ones being exhaled. These small
smoke sized particles will
penetrate a surgical mask. It
would therefore be highly
desirable for everyone to wear
an N95 mask or one with
equivalent or even higher
efficiency.
To achieve this we need to
expand mask and filter media
production. We also need to
improve ways to decontaminate
and reuse masks. H2O2
decontamination methods could
potentially allow a mask to be
reused 10 to 20 times.
Simple mask washing is
the answer for masks made with
nanofibers and
membranes. They
presently account for a
small share of the market. Most
face masks use meltblown media.
McIlvaine predicts that the new
media technologies will
eventually dominate the market.
This will allow individuals to
wash their own masks and not
rely on a decontamination
vendor.
At present meltblown media is
used in most surgical and N95
masks. Meltblown media is also
used in air filters where the
demand is rising rapidly due to
COVID. Together these uses
account for a large portion of
the total.

Face
masks presently account for just
over one fourth of the meltblown
market.
Filtration is a large
application and incudes liquid
filtration, gas filtration,
cartridge filters, and air
filtration for HVAC and
cleanrooms where high efficiency
is required. COVID will increase
the need for meltblowns for air
filters in nursing homes,
apartment buildings,
restaurants, meat processing
plants and many other
establishments where people
congregate. So facemask and
filtration demands will compete
for the limited supply.
Cummins/Dupont are using filter
media normally used in engine
filters for facemasks. The
filtration segment also includes
oil adsorbents.
The
“other” segment includes medical
fabrics such as disposable
gowns, drapes and sterilization
wraps.
Reusable gowns are an
option which would reduce
meltblown demand. Meltblown
fabrics are used frequently in
feminine sanitary napkins,
diaper top sheets and disposable
adult incontinence products.
Also
included in the “other” segment
are disposable
industrial apparel, thermal
insulation and substrates for
synthetic leather. Meltblown
fabrics are sometimes used in
battery separators and as
insulation in capacitors.
If half of the world’s 8 billion
people should be wearing N95
masks and these masks are reused
five times then 800
million masks need to be
produced each day.
N95 masks utilize more meltblown
media than do surgical masks.
|
Mask Production per ton per day of Meltblown Production |
|
|
Mask Type |
Number of masks per ton per day |
|
Surgical |
1 million |
|
N95 |
0.2 million |
World meltblown capacity was
1000 tons per day in January of
this year and has increased as
much as 10 percent over the last
six months.
|
Segment |
Tons per day Meltblown |
Potential # of Surgical Masks per day |
Potential # of N95 Masks per day |
|
Meltblown world capacity as of Jan 2020 |
1000 |
1 billion |
200 million |
|
Sinopec (either or) |
18 |
18 million |
3.6 million |
|
3M 2019 |
15 |
|
3 million |
|
3M 2020 |
30 |
|
6 million |
|
3M 2021 |
60 |
|
12 million |
|
*China 2020-April |
200 |
200 million |
? |
|
China-2020 Jan |
3 |
|
600,000 |
|
World needs -100% N95 |
4,000 |
|
800 million |
|
World needs -100% surgical |
800 |
800 million |
|
*Includes
non meltblown media
Mask production has grown by
triple digits in the last six
months but is not nearly enough
to supply each individual around
the world who congregates with
others each day.
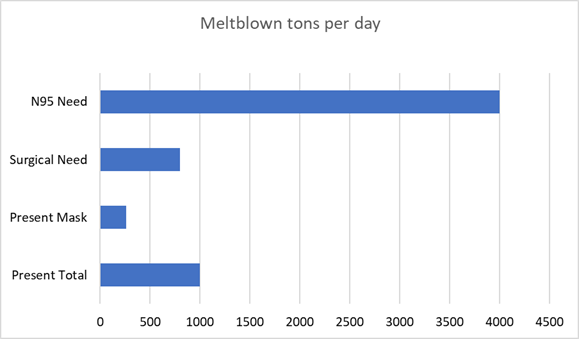
The production of melt blown
media to fulfill the needs of
each person using N95 masks and
replacing them after five uses
would be 4000 tons per day.
This is four times the
meltblown production at the
start of 2020 and more than 15
times the present meltblown
capacity devoted to masks.
However the total is
small compared to the 41,000
tons per day of non wovens
produced for all applications.
So with less than 10 percent
increase in total non wovens
production the media for N95
masks for everyone who ventures
outside each day could be
achieved.
Masks are one of the elements
needed for a safe return to the
new normal.
The
Coronavirus may Become Endemic
like HIV
During a media briefing in
Geneva, Dr. Mike Ryan, executive
director of the WHO's health
emergencies program, warned
Wednesday that the disease may
join the mix of viruses that
kill people around the world
every year.
"This virus just may become
another endemic virus in our
communities and this virus may
never go away. HIV hasn't gone
away," Ryan said. "I'm not
comparing the two diseases but I
think it is important that we're
realistic. I don't think anyone
can predict when or if this
disease will disappear.
"We
may have a shot at eliminating
this virus but that vaccine will
have to be available, it will
have to be highly effective, it
will have to be made available
to everyone and we'll have to
use it," Ryan said. "This
disease may settle into a
long-term problem or it may
not."
WHO
infectious disease
epidemiologist Dr. Maria Van
Kerkhove struck a more
optimistic tone during
Wednesday's briefing."The
trajectory of this outbreak is
in our hands," Van Kerkhove
said. "The global community has
come together to work in
solidarity. We have seen
countries bring this virus under
control. We have seen countries
use public health measures."
Berry Installing New Meltblown
Line in Berlin
Berry Global Group, Inc. announced
the continued expansion of its
global Meltex™ meltblown
capacity, with the addition of
another asset to support the
growing global face mask demand.
This announcement comes as
demand surges due to COVID-19
and the increased need for
nonwoven protection materials.
The new asset is expected to be
operational in October 2020 and
will be placed in Europe at
Berry’s existing production
facility in Berlin, Germany and
will incorporate Berry’s
patented charging technology
post installation. The new line
will focus on the production of
highly efficient filter material
for premium FFP2 (N95) and FFP3
(N99) grade filter media.
“We are now beginning to see the
localization of varying forms of
equipment that produce materials
for PPE, as countries and
governments look to be able to
react with speed to any future
outbreaks,” said Cedric Ballay
EVP & GM for Europe in Health,
Hygiene, and Specialties at
Berry. “We continue to provide
timely solutions to those
looking for assistance fighting
the spread of COVID-19.”
As the largest manufacturer of
nonwoven fabrics, Berry makes
materials for the world’s
leading and emerging brands.
These products range in use from
materials for face masks,
respirators and protective
healthcare apparel to packaging,
many of which have been deemed
essential in the efforts to
fight the spread of COVID-19.
Nursing Homes are Starting to
Incorporate HEPA Filters and
Antimicrobial Coatings
Nursing homes have been
vulnerable to COVID for
multiple reasons. They
include shortages of safety gear
and staff workers who may
inadvertently be carriers and
the design of the buildings.
With shared resident rooms off
long corridors and dining rooms
where everyone mingles, nursing
homes may have been laid out to
be efficient and cost effective.
Since the country’s first
sizable outbreak in a
nursing home in Kirkland, Wash.,
the coronavirus has made its way
into 7,500 long-term care
facilities, killing dozens at
some. Across the country, more
than 143,000 of their residents
and workers have contracted the
illness and more than 25,600
have died, according to
a New
York Times analysis.
That is more
than a third of the deaths from
the pandemic.
Many of the 15,400 nursing
homes across the country
are laid out like hospitals, and
some house hundreds of
residents. Most rooms are double
occupancy, but some have three
or even four residents.
Before the pandemic, a movement
under the banner of “culture
change” was challenging this
institutional model, calling for
dividing up large nursing home
populations into small,
self-sufficient units with
kitchens, private rooms and a
dedicated staff.
Households with private rooms
take up about 10 percent more
space than conventional
interiors with shared rooms and
cost $15,600 more per bed, said
Perkins Eastman, an architecture
firm with an active health care
facility practice.
The
cost of building a skilled
nursing facility in the last 10
years ranged from $223 to $361
per square foot, according to
data based on an index of 100
cities compiled by the National
Investment Center for seniors
and Housing Care, one of the
main data service providers for
the elder care industry.
So
far, an estimated 10 to 15
percent of nursing homes in the
United States are set up this
way. This smaller-is-better
approach arose out of a concern
for residents’ privacy and
dignity, but evidence is
emerging that it may also be
helping with infection control.
A
private room or even an entire
household can be closed off more
easily, keeping out or confining
viruses. Staff members who are
focused on a small number of
residents may be more likely to
pick up on warning signs, such
as a lack of appetite, that
someone is sick. The preparation
of food and laundry in a
household — rather than in
central facilities and then
distributed — also eliminates a
few of the ways diseases can
infiltrate.
The Department of Veterans
Affairs began embracing
a small-house model in 2011;
now, 13 of its 134 nursing homes
are organized around communities
of 10 to 14 residents. In these
settings, only a single veteran
has tested positive for
Covid-19, Christina Noel, a V.A.
spokeswoman, said in a
statement.
Private rooms have made a “huge”
difference in the ability to
control the virus at Jewish
Senior Services, a four-story
building for skilled nursing and
assisted living in Bridgeport,
Conn., said Andrew H. Banoff,
president and chief executive of
the organization. There are 330
residents divided into
households of 14 residents each.
“When somebody is diagnosed,
their door is closed,” Mr.
Banoff said. Signs are posted
and safety gear is placed
outside the door so that staff
know to suit up before entering.
Still, the coronavirus has
cropped up in eight of the 23
households, 15 residents have
died, and four staff members
have been hospitalized, he said.
Administrators of nursing homes
large and small, as well as the
architects who renovate and
design their facilities, expect
to zero in on disease control in
the future as a result of the
pandemic. Air circulation and
filtration will be scrutinized
when heating, ventilation and
air conditioning systems are
planned, they said.
“I’ll be paying more attention
to the HVAC piece of it,” said
John Shoesmith, a Seattle a
architect who specializes in
senior living design.
The Facility
Guidelines Institute,
which writes planning and design
standards that are adopted in
most states and by federal
agencies, set up a task force
this month to make
recommendations for how health
care facilities can cope during
emergencies. Douglas S.
Erickson, the institute’s chief
executive, said the task force
would produce a white paper for
public review by the end of the
summer and publish new standards
in January 2022.
But
some providers are not waiting.
Evermore Senior Living is
wrapping up construction on the
first of 12 small houses for
assisted living and memory care
in Woodbridge, VA. Dave Risi,
the owner operator, said the
first building, which will
contain three households of
eight residents each, will open
in July. Because of the
coronavirus, he is now ramping
up air filtration.
Mr.
Risi already had high-efficiency
particulate air filters,
commonly called HEPA filters,
which can trap bacteria and
other particles. Because of the
coronavirus, he is now adding
ultraviolet light filters that
can kill airborne viruses.
Nursing home providers and their
architects are also talking
about easy-to-clean, nonporous
surfaces; antimicrobial
materials, like copper, for
“high touch” features such as
hand railings; and voice- or
sensor-activated controls for
doors, lighting, curtains,
faucets and toilets.
Even as they battle the
coronavirus, some nursing home
administrators are reassessing
renovation plans that were in
the works when the virus hit.
Andrus on Hudson, a nonprofit
senior care community in
Hastings-on-Hudson, N.Y., had
hired Amenta
Emma Architects to
help with a renovation. Now
James Rosenman, the chief
executive, is talking to the
designers about the possibility
of installing modular walls so
that resident rooms can quickly
be reconfigured in a crisis.
“It’s always been, ‘Do we need
to move the person?’’ Mr.
Rosenman said, referring to how
ill residents have been moved to
isolation areas during the
pandemic. “Maybe we can change
the rooms instead.”
https://www.nytimes.com/2020/05/12/business/nursing-homes-coronavirus.html
UV
Light for Jails and Nursing
Homes
The
Grant County Wisconsin Sheriff’s
Department recently purchased an
ultraviolet light emitter that
staff members use to sterilize
the county jail’s booking area
and holding cells.
The
device recently was lent to the
county’s nursing home, Orchard
Manor, which has experienced at
least 27 COVID-19 infections
among staff and residents.
The
UV light disinfects and cleans
almost every bug and virus out
there,” said Matt Thill, the
facility’s maintenance manager
“We’ve gone down through one of
the wings and disinfected every
room and bathroom, day room,
storage and utility rooms.”
The
device, manufactured by Grand
Rapids, Mich., company Skytron,
emits ultraviolet radiation that
damages the DNA or RNA in
pathogens present on nearby
surfaces, thereby reducing the
chances of infection.
To
prevent injury to users, rooms
must be unoccupied when the
device is turned on.
Onboard sensors on the UV
emitter scan rooms and determine
the intensity of light and
duration of operation needed to
sterilize the area.
The
device, which cost about
$41,000, is small enough to be
loaded onto emergency medical
services vehicles.
Currently at Orchard Manor, 17
residents with COVID-19 are
isolated in a negative-pressure
wing. The wing contains special
air filters that are designed to
prevent the spread of the novel
coronavirus, which causes the
disease.
Orchard Manor staff also
purchased a handheld UV light to
sterilize computer keyboards and
desks along with an ozone
generator that can disinfect
rooms
Washington State Dental Office
will Open with New Air Filters.
For
weeks, the Cannon Hill Dental
office has had a quiet, empty
waiting room. The only people
who came in were people with
dental emergencies.
But
starting May 18, all Washington
dental offices can re-open. Dr.
Amir Ganji, who runs Cannon Hill
Dental, says opening will be a
relief after dealing with the
frustration of being closed.
While
some dental work is not
considered essential, Dr. Ganji
says the lack of consistent
check-ups has caused problems
for some of his patients. He
stressed that the closure has
brought to light how essential
dental care can be.
That's why Dr Ganji is relieved
to open on May 19, the day after
Governor Inslee is allowing all
dental offices to re-open. But
opening a dental office could be
more complicated than opening
other businesses.
"We
are in a field where we generate
aerosol from the mouth, and it
goes into the environment," Dr.
Ganji said. That's exactly how
the coronavirus spreads.
In
order to keep his patients and
his team safe, Dr. Gangi bought
air filters, is doing fewer
procedures that create aerosol,
and has changed his scheduling
procedure. His office will be
seeing less patients than
normal.
Northwestern
Professor looking at Chemically
Treated Masks to Destroy Viruses
Jiaxing Huang, a professor of
materials science and
engineering at Northwestern
University, has
received a $200,000 grant
from NSF to
develop a chemical add-on for
traditional masks that can
destroy COVID-19.
Huang is looking at an
inexpensive way to incorporate
chemicals traditionally found in
sanitation products, which are
known to deactivate a broad
range of viruses. He’s looking
into sprays, as well as
chemically treated fabrics,
patches, and inserts for
disposable or DIY masks—all of
which would ramp up the
effectiveness of existing masks.
“What we need to worry about is
how to fix these agents so they
don’t [release] easily when
people inhale and get into their
lungs,” he says. “But then we
need to have them go away during
exhalation. That’s the science
challenge.”
Ben Gurion University
Researching the Potential for
Electrically Charged Graphene
Chris Arnusch, a water research
professor at Ben Gurion
University (BGU), in Israel,
spent five years developing porous
graphene membranes with
antimicrobial and antiviral
properties for use in water
purification. Now, he’s trying
to validate the technology for
air, with an eye toward adapting
it for masks or air filters.
Pure graphene is an atom-thick
layer of graphite, a component
used in pencil lead, that’s
incredibly strong and conducts
electricity. Arnusch creates a
foam-like form of graphene for
his filters by training a laser
on plastic surfaces. Armed with
seed funding from BGU and the
Israeli government, he’s now
teaming up with a startup to
commercialize this and other
products.
In the case of my water filters,
the pores are larger than the
bacteria and viruses,” says
Arnusch. “But if you electrify
the surface in water, it kills
the bacteria and viruses as they
pass through. I’m trying to see
if it works in the air. Once
proven, we just need to adapt it
to a mask or air filter.”
Graphene also being pursued by
Hong Kong Polytechnic
Laser-induced graphene also
interested Hong Kong Polytechnic
University researchers, who are applying
the material to
disposable surgical masks to
make them self-sterilizing and
ultra water-repellent, so
virus-laden droplets roll off.
In an April paper, they noted
that sunlight could
theoretically sterilize a
graphene-coated mask by heating
it to 176°F.
Carbon Nanotubes are Another
Option
University of Cincinnati
researchers are integrating a
carbon nanotube heater into a
fabric that’s made of carbon
nanotubes and polymer fibers.
The nanotubes’ small diameters
and collective high surface area
could effectively separate
microbes, while heating the
carbon could kill them. Having
successfully applied this carbon
nanotube heater technique to the
water purification industry, the
team is trying to use it to
filter air, with support from
the National Institute for
Occupational Safety and Health,
a division of the Centers for
Disease Control and Prevention.
Masks with Copper Technology
Offered by Multiple Companies
Masks which use copper
technology vary widely in terms
of degrees of effectiveness,
price, and longevity, with some
intended for healthcare use and
others purely as an upgrade from
fabric masks. Costs for single
masks generally run from $10 to
$70, with antimicrobial
properties lasting from 30
washes to the life of the
product. Some companies have
tested their products against
other viruses, though none have
against COVID-19, which requires highly
specialized facilities that
aren’t readily available. “Virus
size, infectivity level, and
chemical properties vary and
influence how well masks work,”
adds Fichtenbaum.
Some high-tech masks come at a
high price, in the $50 to $70
range.
Israeli fiber technology
company Argaman has
one featuring four
copper-infused layers and copper
oxide filters from Czech firm Respilon, which
also sells its own masks.
Israeli startup Sonovia uses
zinc oxide coating and
five-micron filtration that is
supposed to last a year.
Companies that specialize in
copper-infused antimicrobial
apparel and mask specialty
outlets offered more affordable
versions. Copper
Compression and
the U.K.-based Copper
Clothing offer
four-layer masks blocking 99% of
particulates, while Copper
Mask uses
six-ply copper and HEPA filters
blocking 92%. Another company, Kuhn
Copper Solutions—founded
by microbiologist Phyllis Kuhn,
an early
advocate of copper use in
hospitals—specializes
in copper mesh masks and inserts
that can be combined with
traditional or cloth versions.
You can also find copper-infused
cotton masks at some furniture
and apparel outlets—like The
Futon Shop, CustomInk,
and Atoms shoes—that
hopped on the copper bandwagon
by leveraging existing
production pipelines.
